Majority of practice support inquiries come from referrals across all 50-states. Our humble growth from a single doctor / clinic to today’s nationwide support.
In some instances, not all clients’ inquiries for help are immediately accepted. Principal reason is where the practice is not readied to make hard changes which is needed to right the wrongs which is having adverse effect on revenue.
Unlike others in the healthcare space, we are deeply involved in every aspect of billing, from collections to process and practice management. Our success is directly tied to our clients’ success.
Our team includes professionals with backgrounds as Federal Claims auditors and experience with commercial payors such as Cigna, United Healthcare, Aetna, and Blue Cross & Blue Shield.
We also have Practice Administrators who have supported solo doctors, clinics, and Ambulatory Surgery Centers (ASC) in launching or restructuring their internal processes and systems.
Additionally, we excel in pre-authorization and insurance verification of patient benefits, a critical 1st step for practices to ensure payment. We’ve mastered this process, taking the burden off clinics.
Our billing and collection services seamlessly integrate with your current EMR.
- Athena
- eClinical Works
- Aprima
- AdvancedMD
- AllScripts
- ChartLogic
- Dentrix
- EagleSoft
- eMDS
There are many more systems, including all the clearinghouses, to stay updated on claim denials.
Clinical Trials Services
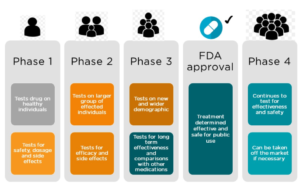
Including clinical trials in a practice setting offers numerous benefits for both the clinic and its patients.
Patients and volunteers benefit from participating in cutting-edge studies that may later receive FDA approval. In many cases, once the study is approved, they can continue to enjoy its benefits for years to come.
The clinic benefits from community exposure to attract new patients and serves as a clinical test site involved in an FDA study.
We’re excited to share that we’re collaborating with one of OKC’s largest pain management clinics to roll out a clinical trial module.
By FY-2025, we expect to launch our first trial, with the capacity to conduct 3 to 5 trials in the first year.
Reach out to one of our Medical Advisors to see if your practice qualifies as a Clinical Trial Site: 214-797-6170.
Cardiac News
CV Highlights From the 2025 Hospital OPPS Final Rule
The Centers for Medicare and Medicaid Services (CMS) released the 2025 Hospital Outpatient Prospective Payment System (OPPS) and Ambulatory Surgery Center (ASC) final rule on Nov. 1. The rule will implement a 2.9% increase to OPPS payment rates that reflects a market basket update of 3.4% reduced by a productivity adjustment of 0.5%.
">CV Highlights From the 2025 Hospital OPPS Final Rule - American College of Cardiology
A new enhanced benefit feature is now available: Procedure Code Look-up For Health Care Providers June 2021
UNITED HEALTHCARE WILL DENY OR LIMIT COVERAGE FOR ED COMMERCIAL CLAIMS IT CONSIDERS NON-EMERGENT

Our skills covers all aspects of dental care:
- Pre Authorization
- Insurance Verification
- Insurance Billing – Charge Entry
- Collections to Patient Statements
- Bookkeeping and payroll services
- Dental credentialing to Practice Admin services
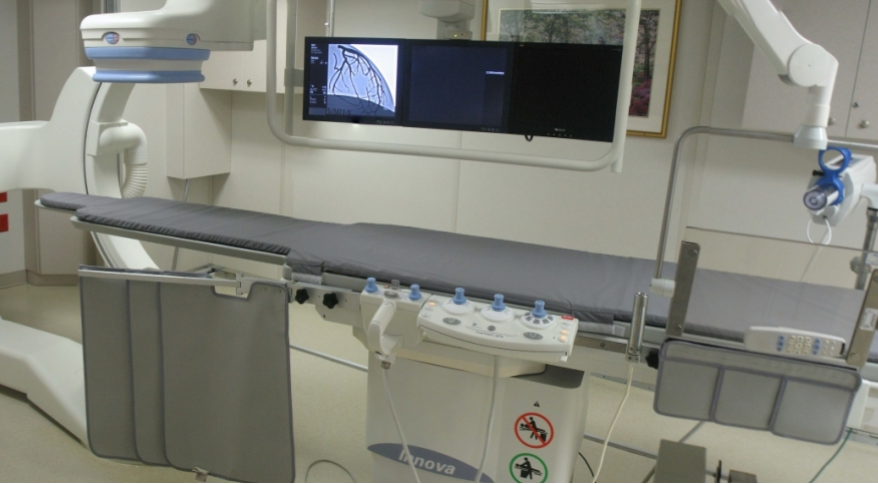
ASC and Cath Lab Developments
We work closely with seasoned talents whose knowledge in ASC and Cath Lab facilities will significantly reduce development cost.
Including credentialing the facility – provider and subspecialties before the facility is readied for 1st patients.

Pre Auths for Surgery & Meds
When Prior Authorization are Delayed, Patients Suffer
We Handle Medical Authorizations to Save You Time and Drive Outcomes. Pre-authorizations Are Mandatory. Waiting On Hold Is Optional. Let Us Take It On For You. Network-Enabled Services. Services for Hospitals. 24/7 Support

Insurance Verification
Patient insurances are changing monthly. And in most cases; patients do not have an idea what their plan covers, much less how much is out of pocket available per their deductible. We handle this for many practices across the country.
Next, this process takes up valuable staff time. We customize our process to each clinic needs. The information captured is entered in the clients own EMR.

Credentialing Services
Credentialing is one of the most important aspect of keeping the clinic and providers current with payors contracts. Facilities – Doctors – NP-C -CRNA and many more.
We work the whole process from CAQH, to Availity and setting up EFT payments directly to the provider’s bank account.

Facility & Provider Fee Schedules
A fee schedule is a complete listing of fees used by Medicare to pay doctors or other providers/suppliers. This comprehensive listing of fee maximums is used to reimburse a physician and/or other providers on a fee-for-service basis.
Cigna, Humana, Aetna and others issue the following year fees schedules for all disciplines in healthcare. CMS, also issues their fee schedule. All of which needs to be uploaded in your EMR.

So, my husband owns several Bariatric Clinics in New York & New Jersey; we invited Gabriella, to audit our Billing process. Her findings were very effective. And since have made internal changes to bring the money.

Hired Chris, as BOM for our new ASC here in Kingwood. Within 6-months Chris got us on all of the major commercial plans. Highly recommend to anyone who needs amazing help! Now, we can see commercial payors patients. BCBS, Aetna, Cigna, Superior Health, United Healthcare, and Humana.

Gabriella is always responsive to my late text pertaining to surgeries and coding. "She's a machine," no other way to explain how effective and quick she is. Routinely, I have called upon her still, for a question or two. Happy to have gotten to know her. We use Athena & pMD, she remotes in drops the claim correctly, without telling her. A surgeons dream to have her on your billing team.

I have worked with Chris when he was at Oklahoma Eye Surgeons as Practice Administrator. He's very organized and easy to work with. Excellent with patients and fellow team members. Goes way out of his way to keep business running smoothly. I noticed major improvements within the 1st month.
Medical Billing Software and Clearinghouse Partners








